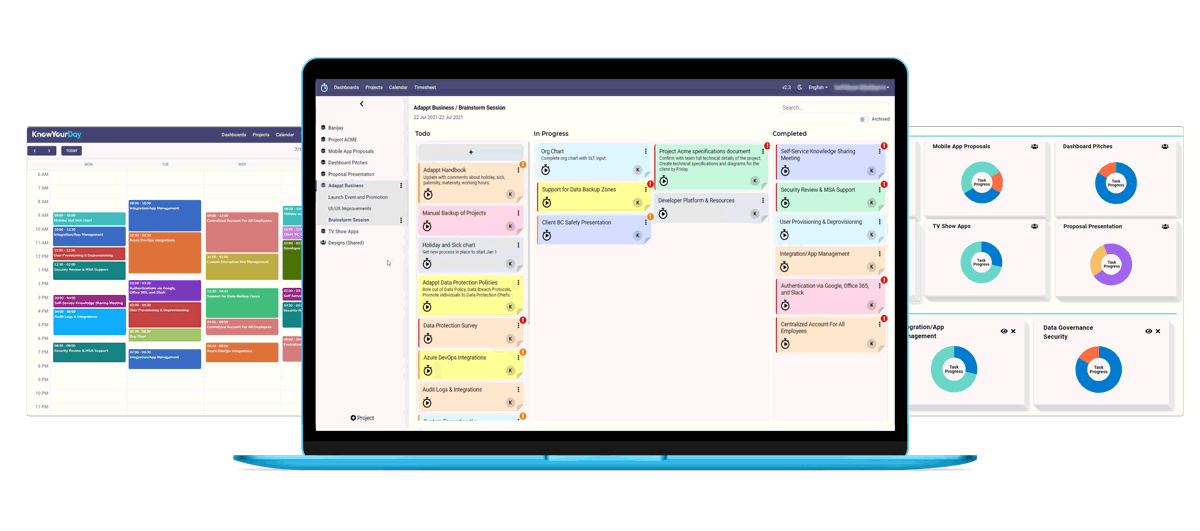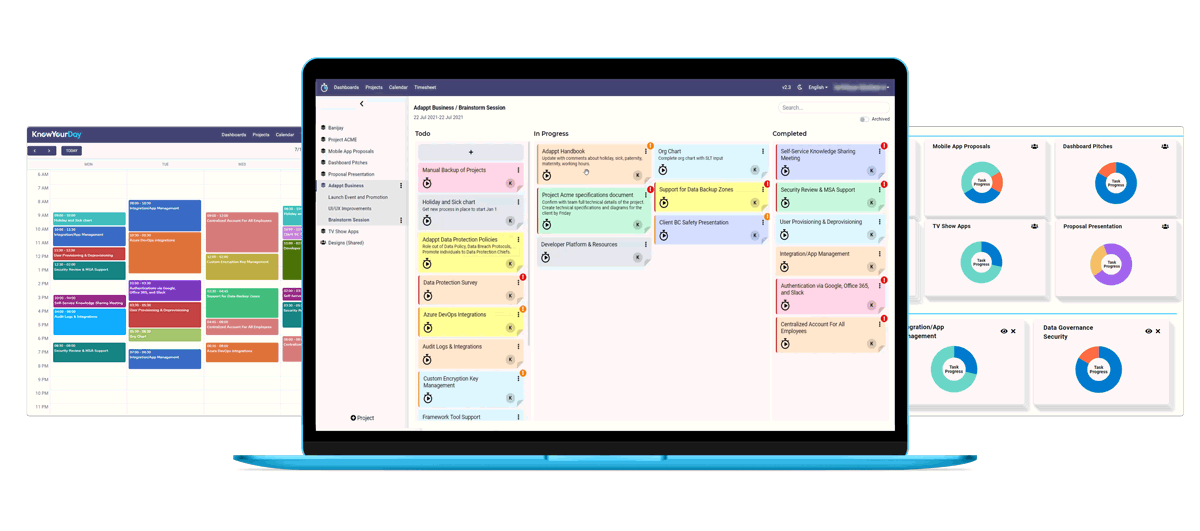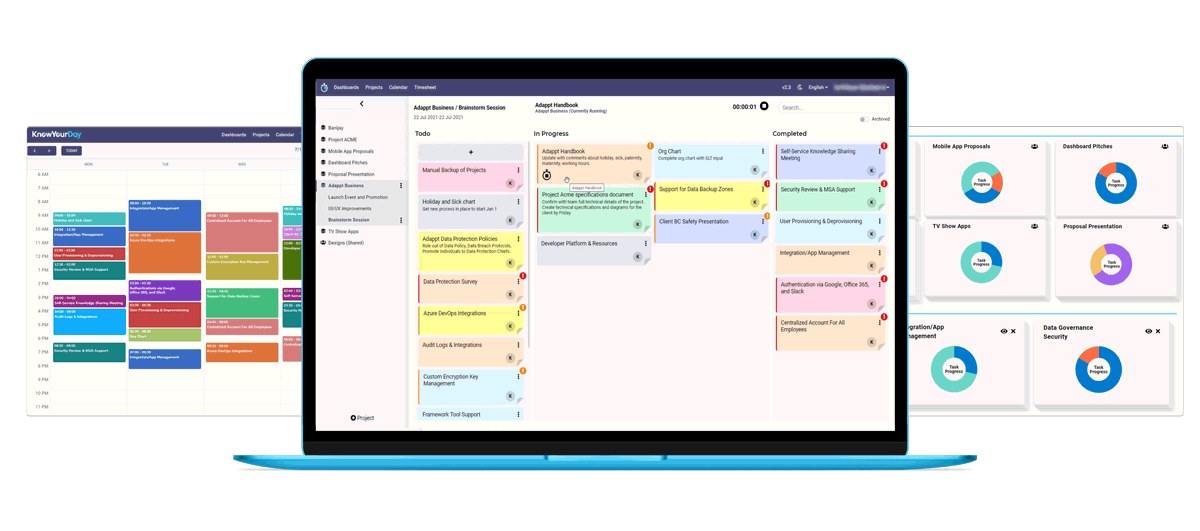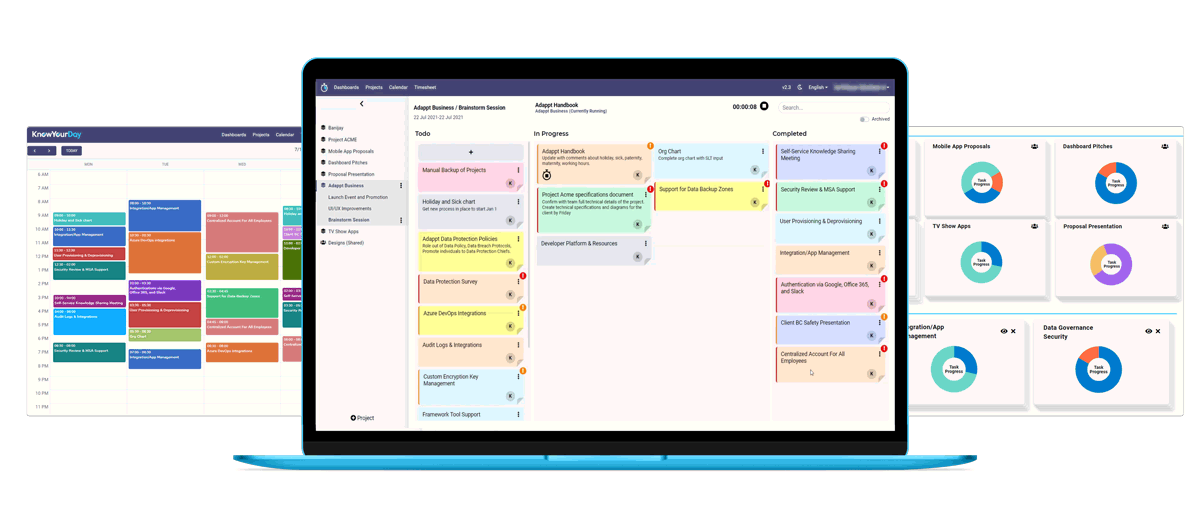
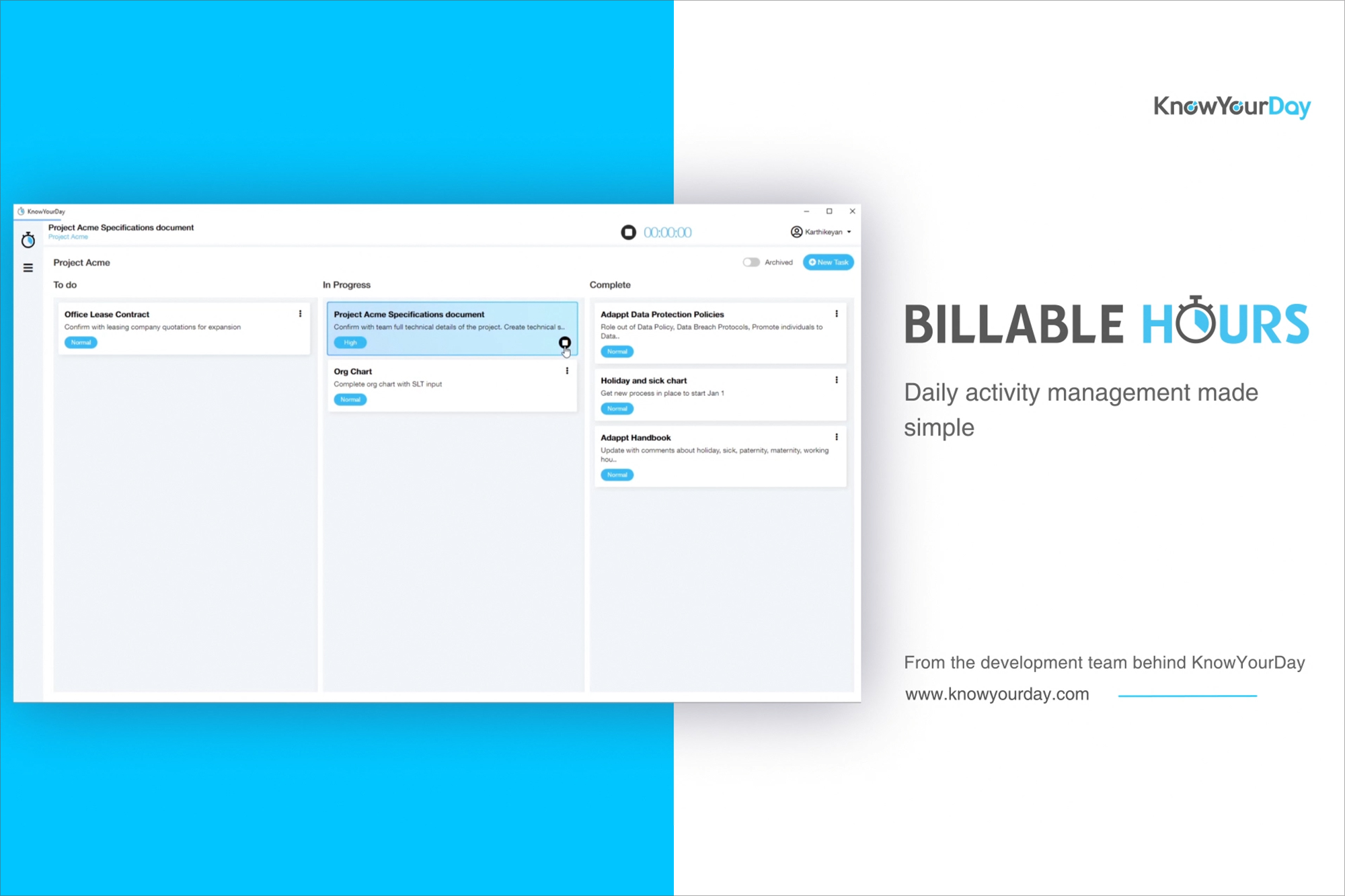
Cronus from KnowYourDay is the new user friendly pop-up app that helps you manage your projects daily whilst tracking the time spent on each of them across your whole workday.
Easily create projects and tasks you want to track, and Cronus will compute the time spent on each in the background.
So if you are an entrepreneur, consultant, freelancer or a designer, try out the new KnowYourDay Cronus time tracking app for your next project.
KnowYourDay is a new simple employee productivity solution and the time tracking tool that both you and your staff will like using. It contatins everything you'll need to improve the effectiveness of your remote staff and develop your organisation remotely, all while protecting user privacy.
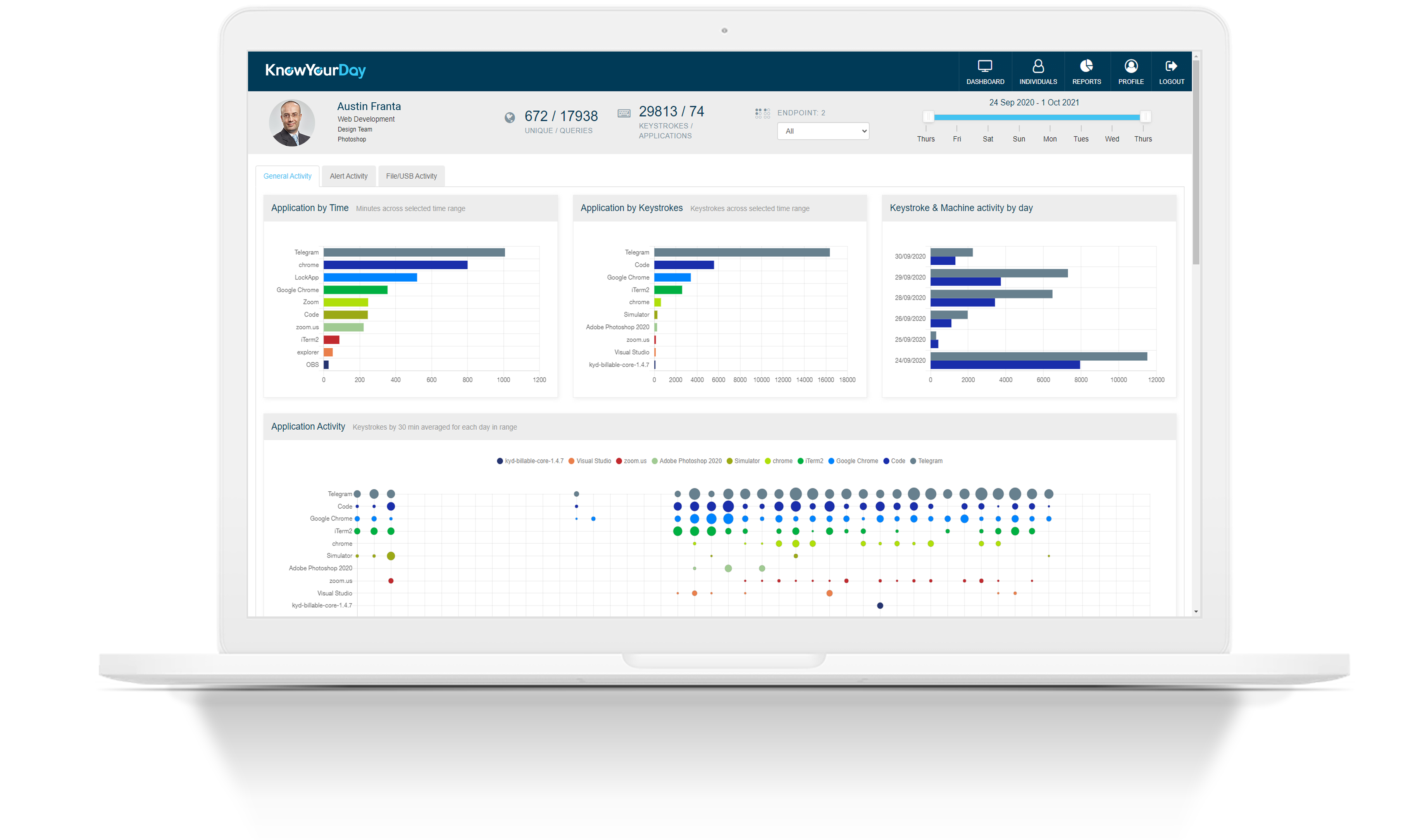
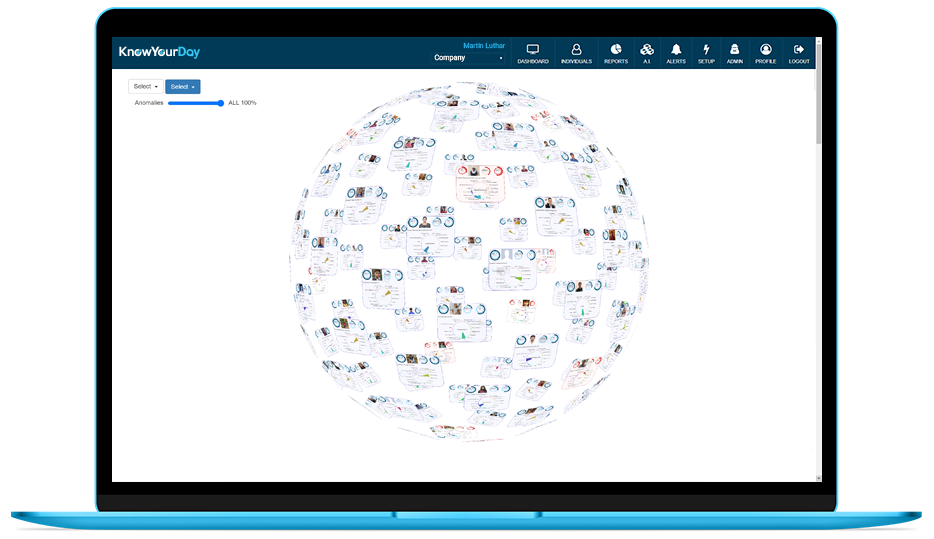
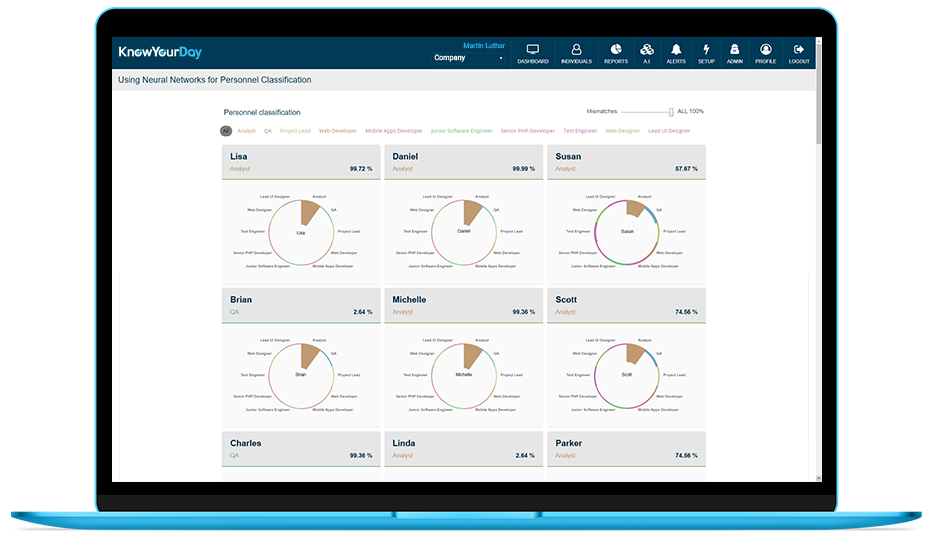
KnowYourDay provides an instant picture of your company’s overall performance. See how staff are working in real-time, where the business is focused, where time is spent and on which applications.
KnowYourDay is the ultimate remote workforce platform, providing you with the information you and your teams need to manage the business remotely.
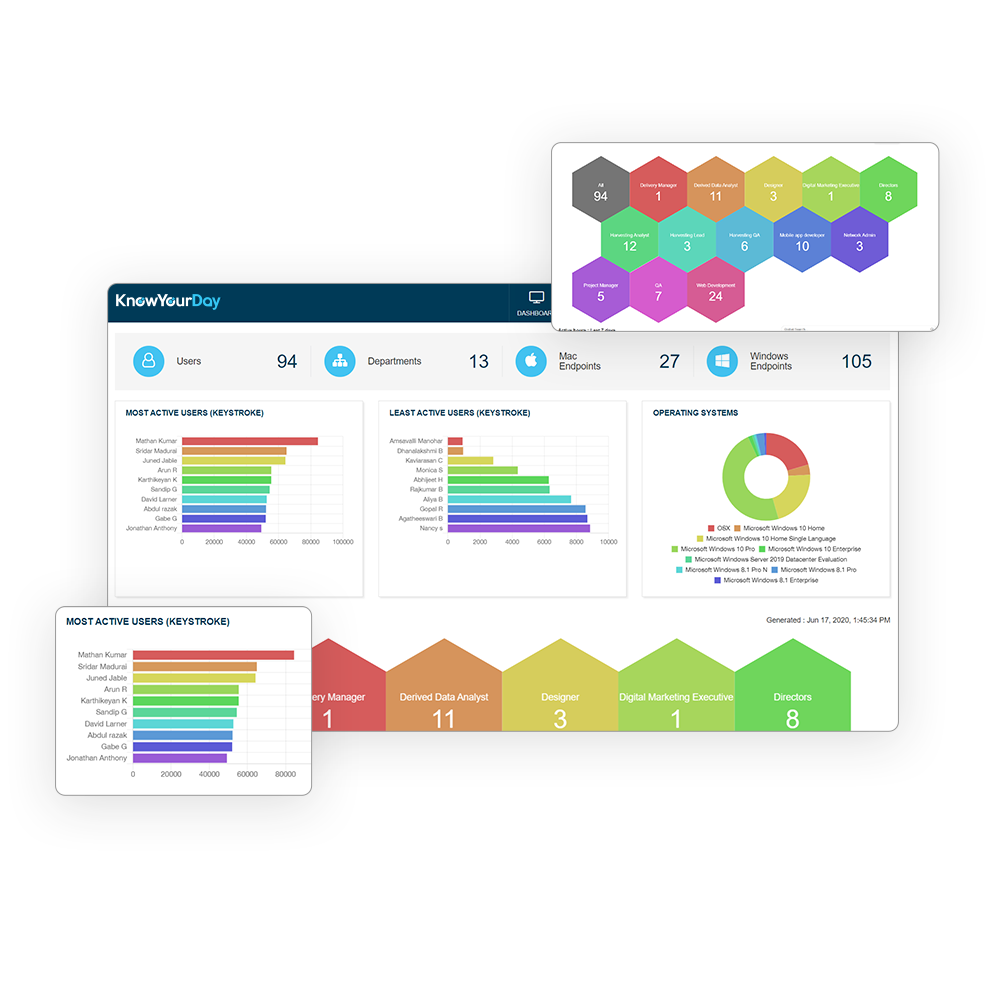
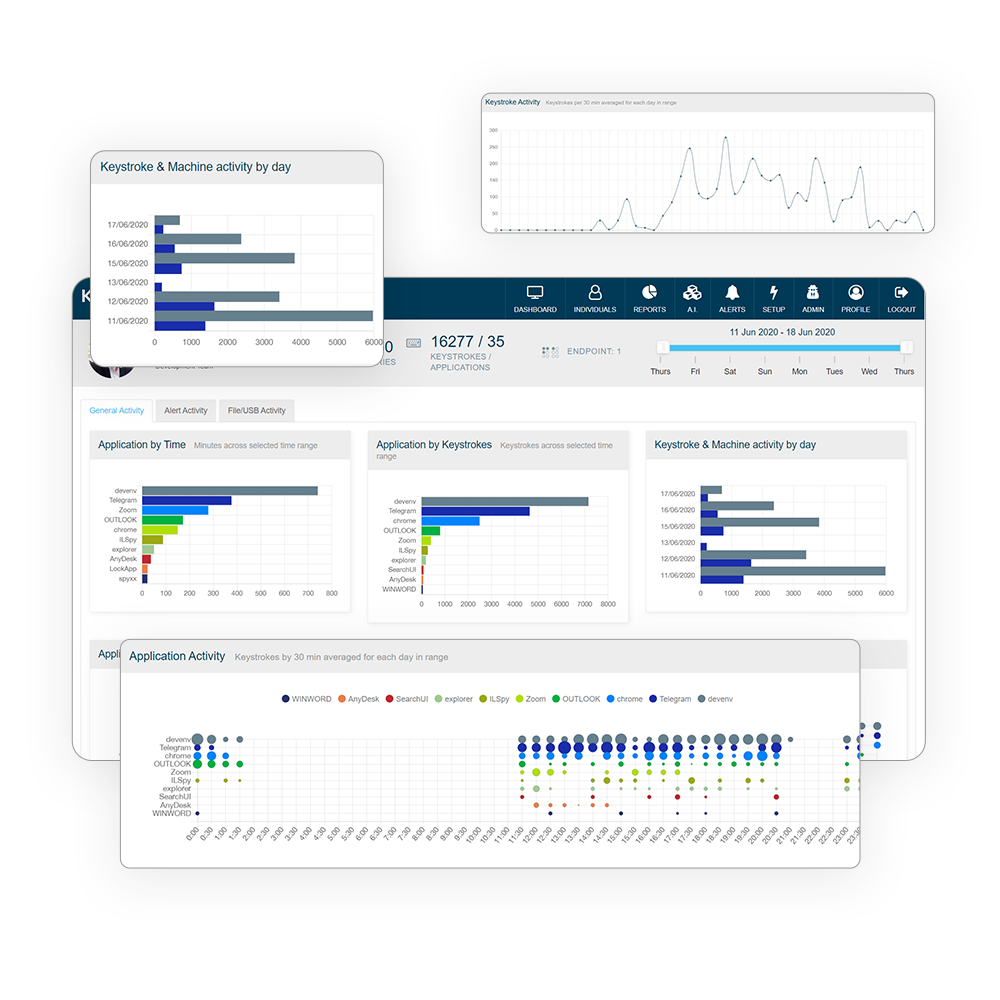
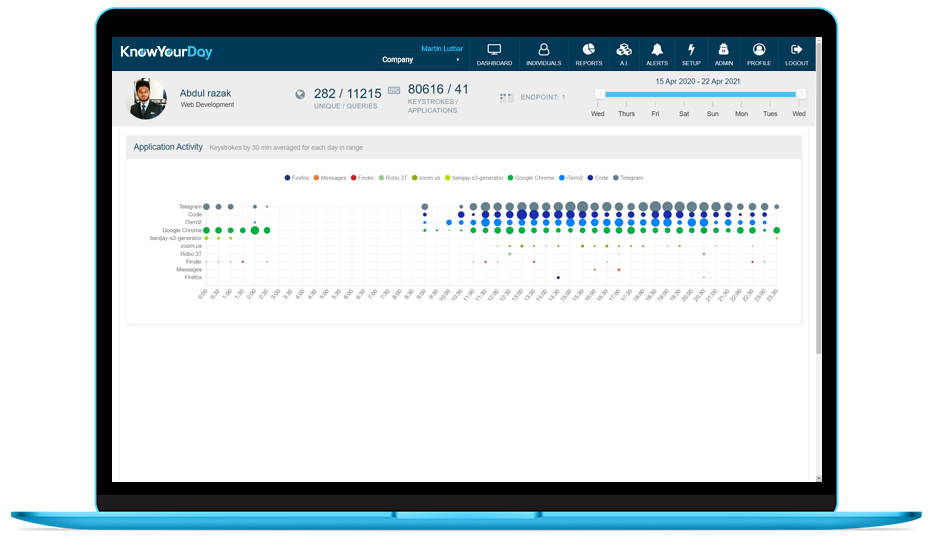
Whether you choose by team, department or individual, our activity charts give you lightning fast views of overall activity from daily, weekly and customisable views.
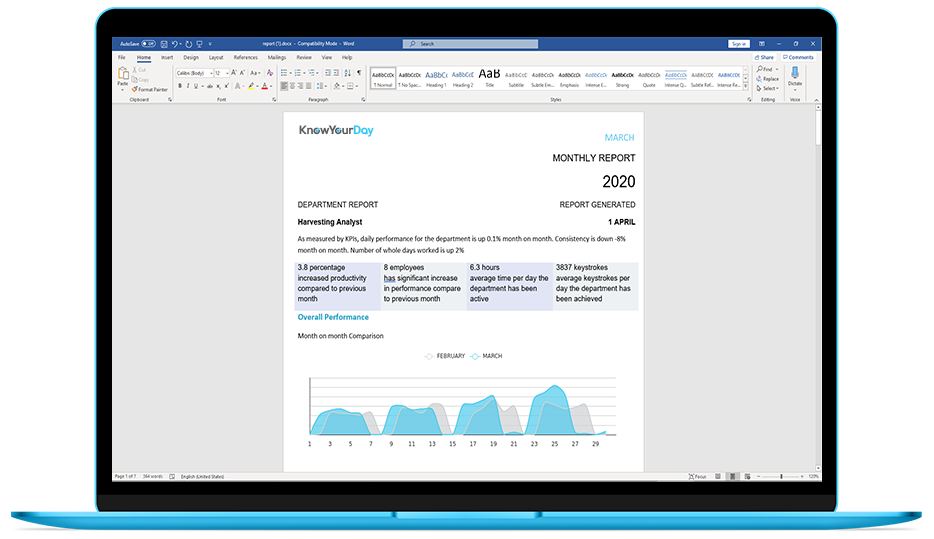
Users will gain really insight as to how their time is spent, where their focus is and learn where they can reap rewards to improve productivity. Our Day-to-day views show:
User privacy sits at the heart of KnowYourDay. Unlike other tools, we don’t need to collect personal information to provide you with the business metrics you need, meaning greater transparency and adoption across your network.
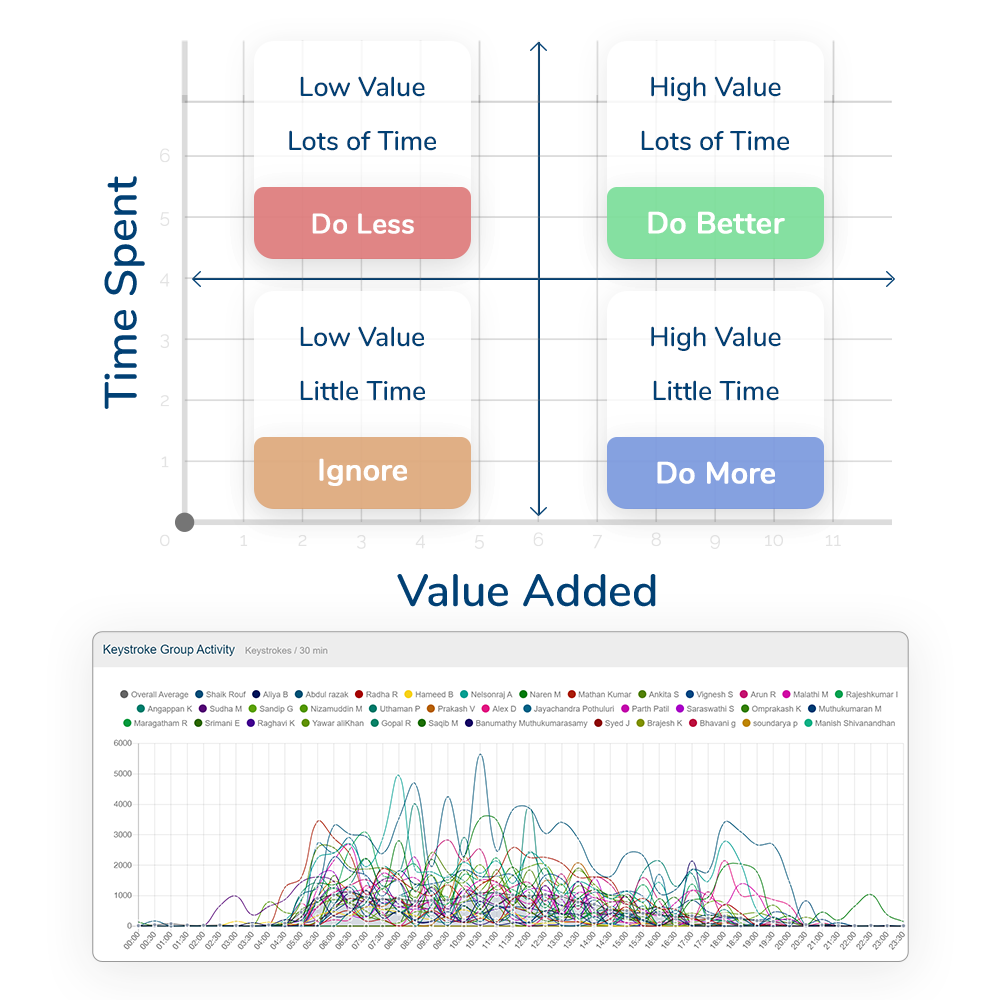
KnowYourDay’s helps you identify where time is being spent around the business and which are the areas that deliver very little.
By reducing time spent on low value tasks (or eradicating them altogether) you can vastly improve productivity by freeing up time for what’s important.
KnowYourDay’s helps you to:
Did you know that on average we generate around 50,000 data points during a typical workday?
Whilst individually these are meaningless, put together, they create valuable insight into user behaviours, skills and patterns of work that can enhance your business.
That’s where KnowYourDay’s powerful AI engine comes in.
By getting to understand users, KnowYourDay can help flag variations in behaviour that may signal something important to the business.
KnowYourDay’s AI gives you valuable insight that you otherwise wouldn’t have across your remote workforce. Employees benefit hugely from having an accurate record of their work efforts supporting them during remote working.

Spoiler alert: You DO NOT need to collect sensitive user information to manage remote workers!
We make no apologies:
KnowYourDay is designed and architected as a productivity improvement tool, not a ‘snooper’ device, personal privacy is a priority.
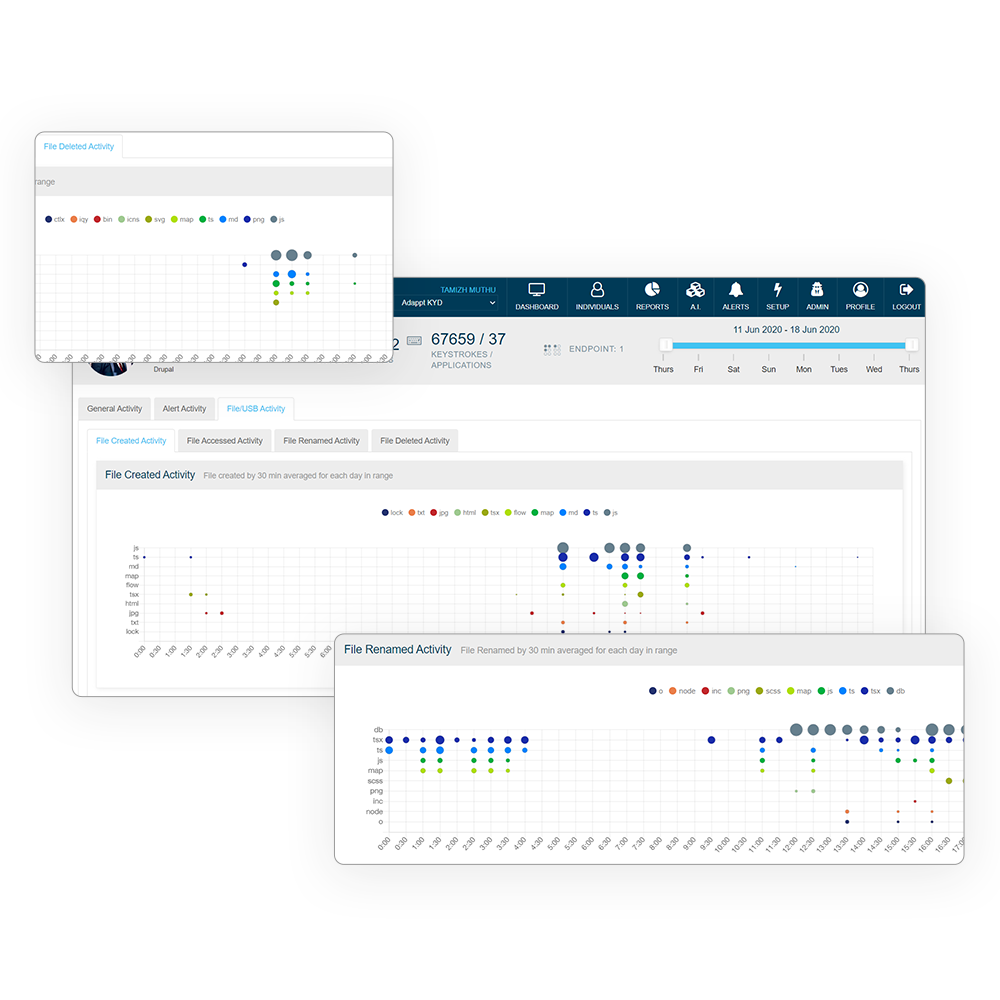
It’s an unfortunate reality, but most cyber-crime happens from within. KnowYourDay has built in security features which can be tailored to protect your companies data, trigger access alerts, log nefarious actions, and tools to make you aware if you have potentially been hacked. Alerts include:
Being light-touch, our focus is on user privacy, but where suspicious activity is happening across your network, we feel you’d like to know. As with all our features this can be customised to suit your requirements.
Start working with KnowYourDay today. It’s simple to install and can be up and running in minutes.
To learn more about KnowYourDay and the Cronus Productive Suite, view our walk-through videos below:

Choose from simple cloud downloads to customised / on-premise installation. KnowYourDay is flexible to suit whatever your business requirements.
Keep accurate track of your time, projects and tasks.
Cronus, All the Task, Project and Time Features Plus Export with controllable rates by contract or task.
Digital Time and Motion Study Suite for Today's Distributed Workforce.
Want to know more or talk with a member of our team?
We’d love to hear from
you!
Start working with KnowYourDay today – It’s fast, it’s simple, it’s remote working at it’s best!
3 Ilex House, 94 Holly Road, Twickenham, TW1 4HF